 The ankle joint is stabilized by different ligaments and other soft tissues, which may also be injured during an ankle fracture. An ankle fracture is a painful condition where there is a break in one or more bones forming the ankle joint. Pain after ankle injuries can either be from a torn ligament and is called an ankle sprain or from a broken bone which is called an ankle fracture. 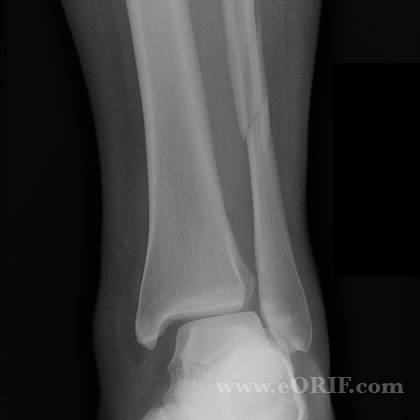
What is an Ankle Fracture?Īnkle injuries are very common in athletes and in people performing physical work, often resulting in severe pain and impaired mobility. The joint is protected by a fibrous membrane called a joint capsule, and filled with synovial fluid to enable smooth movement. The ends of the fibula and tibia (lower leg bones) form the inner and outer malleolus, which are the bony protrusions of the ankle joint that you can feel and see on either side of the ankle. The ankle joint is composed of three bones: the tibia, fibula, and talus which are articulated together. Kono T, Ochi M, Takao M, Naito K, Uchio Y, Oae K (2002) Symptomatic os subfibulare caused by accessory ossification: a case report.Ankle Fracture What is Normal Ankle Joint Anatomy? Griffiths J, Menelaus M (1987) Symptomatic ossicles of the lateral malleolus in children. 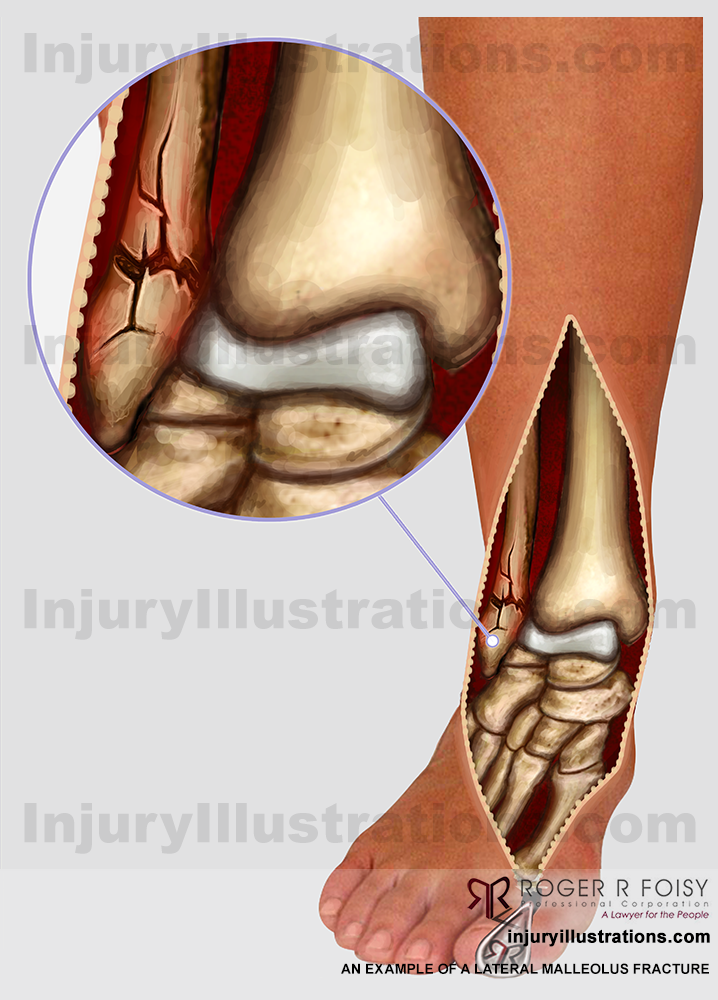
Hasegawa A, Kimura M, Tomizawa S, Shirakura K (1996) Separated ossicles of the lateral malleolus. Mellado J, Ramos A, Salvado E, Camins A, Danus M, Sauri A (2003) Accessory ossicles and sesamoid bones of the ankle and foot: imaging findings, clinical significance and differential diagnosis. Powell H (1961) Extra centre of ossification for the medial malleolus in children: incidence and significance. Ogden J, Lee J (1990) Accessory ossification patterns and injuries of the malleoli. 
Avulsion fracture of the fibula associated with recurrent instability of the ankle. 41-63īerg EE (1991) The symptomatic os subfibulare. Sports injuries in children and adolescents Berlin, Springer, p. Vanhoenacker F, de Cuyper K, Williams H (2011) Normal anatomy and variants that simulate injury. Excision of the os subfibulare should be reserved for patients with recurrent sprains and persistent pain. To assist the differential diagnosis, os subfibulare has a round shape and smooth, well-defined cortical margins, whereas an acute malleolar avulsion fracture fills the missing part of the distal tip of the lateral malleolus, with irregular cortical margins facing the fibular tip.Īsymptomatic patients can be treated effectively with immobilization, anti-inflammatory agents, physiotherapy and modified footwear. No contrast medium was administered to the patient to investigate injury.ĭespite its rare occurrence, it is important to distinguish os subfibulare from an acute avulsion fracture of the lateral malleolus to avoid delayed fracture diagnosis that may lead to complications as malunion, nonunion, or a chronically painful ankle. In this case, the uppermost fragment of the ossicle was of abnormal low signal intensity on T1-weighted MR images with corresponding high signal intensity on T2-weighted and STIR images, indicating bone marrow oedema due to post-traumatic fracture. The latter are commonly caused by inversion injuries in the clinical setting of ankle sprains. Furthermore, the ossicle may cause limitation of the range of motion of the ankle joint resembling avulsion fractures of the lateral malleolus. Mechanical irritation or joint instability may cause pain and recurrent ankle sprains. It has been postulated that symptoms are associated with disruption to the fibrous or cartilaginous attachments of the ossicle resulting in a fracture, fibrous union, or pseudarthrosis. Ossicles may also be connected to the fibres of the posterior talofibular ligament. Arthroscopic and operative findings have shown that os subfibulare is embedded partially or completely within the fibres of the anterior talofibular ligament, with some parts exposed in the talofibular joint or covered by a synovial membrane. The os subfibulare most commonly remains asymptomatic, however, it may cause pain, sustain or simulate a fracture, or it may even precipitate arthrosis in response to overuse and trauma. The os subfibulare is usually round, oval, or comma-shaped. Such ossicles rarely persist beyond skeletal maturation with a reported prevalence of 1- 2.1%. It appears toward the end of the first year of life and fuses with the metaphysis between the ages of 15 and 17 years. The ossicle is located under the tip of the lateral malleolus. The os subfibulare is a normal anatomic variant that represents either an unfused accessory ossification centre or a supernumerary bone. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
